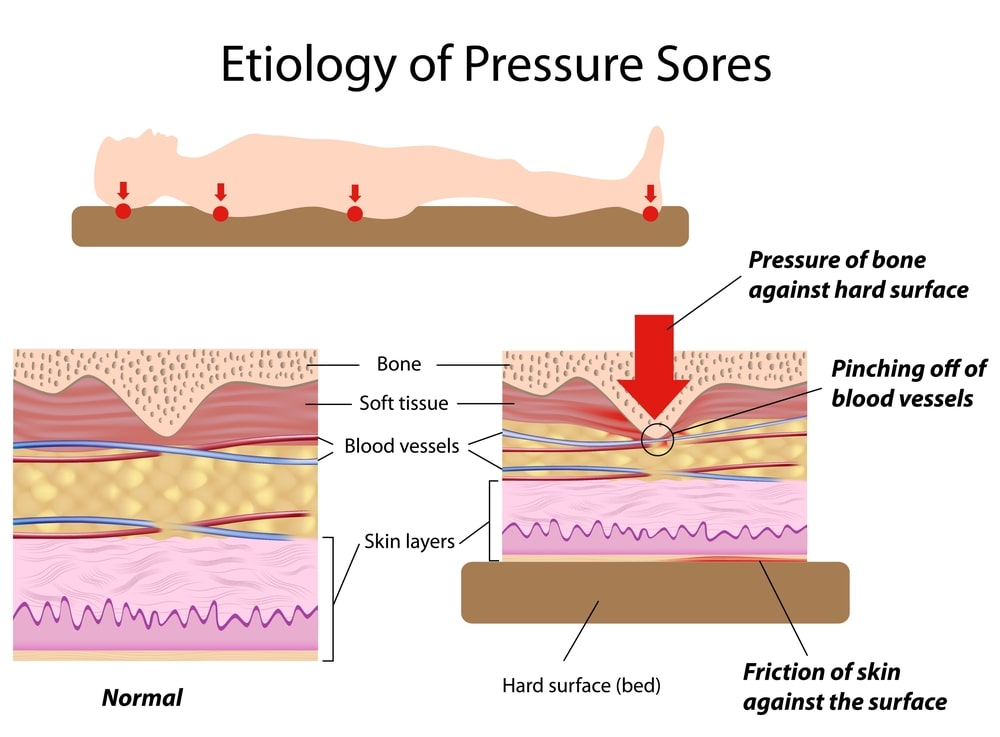
Pressure sores, or bedsores, occur when immobile patients spend long stretches in bed and are unable to relieve the pressure on parts of their body that make contact with the bed. It happens most often in areas where the skin is close to the bone. If someone you love resides in a nursing home or has an in-home caregiver, be on the lookout for one sure sign that they are not receiving the care they deserve.
Table of Contents
What Causes Pressure Sores in Elderly Patients?
There are three primary causes of pressure sores:
- Friction
- Shear
- Sustained pressure
Each is discussed further in the following sections.
Friction
Friction occurs when the patient changes positions or moves from a bed to a wheelchair. The skin rubs against another surface, such as the bed sheet or clothing, and the other surface resists the applied motion. Repeated exposure to this movement can lead to friction sores, which weaken the skin and increase the risk of pressure sores.
Shear
Shear is another primary cause of pressure sores in elderly individuals. It is similar to friction, except the two surfaces are moving in opposite directions. Shear can damage tissue and blood vessels, and make the skin more susceptible to the third cause of pressure sores: sustained pressure.
Sustained Pressure
Sustained pressure occurs when an inactive patient’s skin and tissue become trapped between two hard surfaces:
- Bone, and
- A resting surface, such as a wheelchair or bed
The resulting pressure may be enough to prevent adequate blood flow from reaching the area. Without proper blood flow (and the oxygen and nutrients it carries), skin tissue can eventually wither and die. Understanding what causes pressure sores is essential to preventing them and ensuring proper care for elderly patients.
Shear vs Friction
Understanding shear vs friction is important when evaluating how pressure sores develop in elderly patients. Although both contribute to skin damage, they occur under different conditions and require different preventive approaches.
Friction is typically associated with direct contact between the skin and an external surface, especially during repositioning. It mainly affects the outer layer of the skin and can lead to gradual breakdown over time. In some cases, repeated rubbing may lead to minor skin damage, often referred to as friction sores.
Shear, however, is more closely related to body positioning and gravity. It often occurs when a patient is positioned at an incline and begins to slide downward. In this situation, the skin may remain in place while deeper tissues shift, creating internal stress and damage.
Recognizing the difference between friction vs shear helps caregivers take appropriate steps to reduce both surface-level injury and deeper tissue damage.
| Factor | Friction | Shear |
|---|---|---|
| Primary trigger | Skin rubbing against surfaces (e.g., sheets, clothing) | Body sliding or improper positioning |
| Where it acts | Outer skin layer | Underlying tissues beneath the skin |
| How it develops | Repeated rubbing or dragging | Opposing movement between skin and deeper structures |
| Visibility | Usually visible early | May not be immediately visible |
| Prevention focus | Reduce rubbing and pressure points | Maintain stable positioning and support |
Where to Look for Pressure Sores
Some of the common spots for pressure sores in elderly, bedridden individuals include the following:
- Hips
- Elbows
- Ankles
- Heels
- Back
- Spine
- Shoulder blades
- Sides and back of the head
Pressure sores in elderly patients who spend a lot of time in wheelchairs are also common. Whenever someone spends a lot of time in one spot, bedsores are a risk.
The 4 Stages of Pressure Sores in Elderly Patients
In the early stages, minor skin damage may begin to appear, sometimes starting as friction sores, before developing into more serious pressure injuries if left untreated. Bedsores, if not treated immediately, can increase in seriousness through four stages:
- Stage 1 – Skin is intact, but discolored and painful
- Stage 2 – The wound opens, or looks like a pink blister filled with fluid
- Stage 3 – Sores become deep and craterous; infection spreads
- Stage 4 – The wound is so bad that bone, tendon, or muscle tissue becomes exposed
How to Treat Pressure Sores in Elderly Patients
Bedsores can be prevented by encouraging patients to change positions, lay on different sides of their bodies, and move from a bed to a wheelchair. However, if it is too late, due to caregiver neglect or patient obstinacy, there are several ways to treat pressure sores.
- Keep the wounds clean with cleaning solutions
- A course of antibiotics
- Reposition the patient often
- Use specially designed pillows, mattresses, or cushions
Conclusion: Pressure Sores in Elderly
If your loved one is suffering from stage 3 or 4 bedsores while in the care of an in-home nurse, an elder care home, or even a relative, the odds are substantial that something is very wrong with the care the patient is receiving. It might be a good idea to change services or homes, and perhaps even to seek legal counsel on the patient’s behalf.
If you suspect a loved one has been injured, neglected or abused while in the care of a Southern California nursing home, assisted living facility or caretaker, or if you are the victim, it is important to contact Moran Law immediately to discuss your case.